Emergency Landing In Dallas After Scuba Diver Gets Sick
CBS DFW
A couple returning home from their honeymoon in Cancun, Mexico had to make an emergency stop in Dallas after the groom suffered severe decompression sickness mid-flight.
https://cbsloc.al/323JowB
A plane had to make an emergency landing in #Dallas because a man needed life-saving treatment. He had been scuba diving and suffered from decompression sickness. Learn how the #HyperbaricMedicine Unit at Texas Health Dallas helped care for the diver. https://t.co/ELYyhhWZ1F pic.twitter.com/5mELJcIjcJ
— TexasHealthResources (@texashealth) July 17, 2019
TEXAS HEALTH
A flight from Mexico to Colorado was diverted to Dallas when a man suffered decompression sickness and needed life-saving treatment.
Malik Altoos and his wife Kenda Albaree were on their way home to Denver from their honeymoon in Cancun when Altoos started feeling sick.
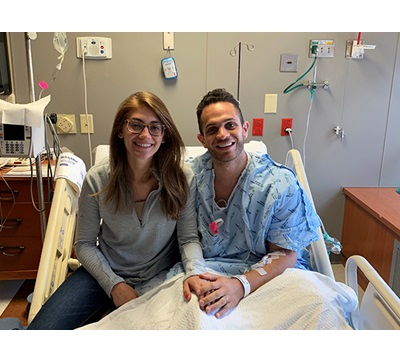
“We were only about 20 minutes into the flight when my hands started tingling. I felt nauseous, dizzy and had trouble breathing,” Altoos said.
Altoos woke up his wife and flagged down the nearest flight attendant. Having gone scuba diving during the trip, he was worried about decompression sickness (DCS), also called the Bends. It’s a rare but potentially fatal condition if divers stay under water too long or rise too quickly to the surface. Flying in an airplane soon after diving can increase a person’s chance of suffering from the condition.
“I told the flight attendant, ‘I need oxygen right away. I think I have decompression sickness,’” said Altoos, who is 26-years-old.
Altoos and his wife went to the back of the plane where he was given oxygen. Two internal medicine doctors, who happened to be on the same flight, monitored his vital signs — pulse rate, breathing rate and blood pressure. As the oxygen tank was getting low, the physicians told the flight attendant to notify the pilots about making an emergency landing.
“I was trying to stay calm because I had no other option,” Altoos said. “I honestly didn’t think I was going to make it through the flight.”
Despite the unknown outcome, he looked to his wife for comfort and guidance.
“I kept telling him to breathe and tried to reassure him that everything was going to be okay,” Albaree said.
Beneath the surface
The newlyweds and recent dental school graduates spent a memorable week in Cancun where they enjoyed swimming, playing beach volleyball and scuba diving. They went on three dives — from 15 feet to 30 feet below the surface. The couple says they had no issues. Then 19 hours after the couple’s final dive, they boarded the flight home.
“He had been working out a lot which made him very dehydrated,” said Edward Tomoye, D.O., an internal medicine and infectious disease physician on the medical staff at Texas Health Presbyterian Hospital Dallas.
People who do high intensity workouts before a dive increase their risk for decompression sickness, said Tomoye, who also specializes in undersea and hyperbaric medicine. The illness results from the reduction in the ambient pressure exerted on the body during ascent from a deep or lengthy dive which can cause expansion of nitrogen bubbles in tissues. It occurs in 1,000 U.S. scuba divers each year, according to the Divers Alert Network.
On the surface of the earth, we breathe in a greater percentage of nitrogen than oxygen. At this normal atmospheric pressure, the body processes the nitrogen fine, but it can become dangerous when scuba diving.
“When you go diving, the laws of physics take over. The deeper you dive, and the longer a diver stays immersed, the nitrogen bubbles in your blood stream dissolves and it’s stored in various bodily tissues,” Tomoye said. “If you come back up to the surface rapidly or you stay in the water for a long period of time, those bubbles expand and block blood flow.”
Tomoye says it’s like bubbles in a soda can. When you open a can, the dissolved bubbles or gas has a chance to release slowly because of the gentle reduction in pressure. If you shake the can, it will release the liquid quickly with formation of multiple bubbles.
Altoos still had nitrogen bubbles in his body when the plane reached 35,000 feet, making it hard for him to breathe.
“The oxygen on the plane saved his life,” said Tomoye. “It helped flush out the extra nitrogen.”
Back on solid ground
The plane landed safely in Dallas and several hours later Altoos was brought to the Emergency Department (ED) at Texas Health Dallas. Tomoye did a neurological assessment on Altoos and determined he needed hyperbaric oxygen therapy as soon as possible.
The hyperbaric medicine unit is part of the Institute for Exercise and Environmental Medicine at Texas Health Dallas. The joint program between Texas Health and UT Southwestern Medical Center promotes clinical research, clinical practice and human physiology education. It’s the only Texas Health facility that offers hyperbaric oxygen treatment for critical care patients. It’s the largest multi-place hyperbaric unit in North Texas.
The IEEM’s hyperbaric oxygen therapy infuses 100 percent oxygen at pressure levels that are two to three times greater than normal. The high oxygen pressure allows the lungs, body fluids and tissues to absorb oxygen. This process promotes and accelerates healing. The chamber is pressurized with air. Patients wear either a mask or see-through vinyl hood/helmet that is connected to tubes — one for oxygen and one to remove carbon dioxide.
In addition to decompression sickness, hyperbaric oxygen therapy helps patients with complications from radiation treatments, skin grafts, diabetes, surgical incisions, trauma wounds, as well as carbon monoxide poisoning, sudden blindness and hearing loss.
Altoos had three treatments, over the course three days, in the hyperbaric chamber.
“Within 10 minutes he was looking and feeling better,” said Adam Mottley, C.H.T., a safety officer on the hyperbaric medicine unit. “We noticed a big difference after the first treatment.”
Plan your dive
Experts say people should be mindful of the potential problems and dangers that could arise on a dive.
“Plan your dive and dive your plan,” Mottley said. “You wouldn’t climb Mount Everest without the proper training and gear. The same goes for diving.”
If you do a single dive one day, Tomoye recommends you wait at least 12 hours before taking a flight. If you’re doing multiple dives in one day — which Altoos did — you should wait at least 18 hours, and preferably 24 hours before boarding a commercial aircraft.
“I’m so grateful for the phenomenal care at Texas Health,” Altoos said. “They were sympathetic and went out of their way to help me and my family. I want to carry that on with my own patients.”
https://www.texashealth.org/Newsroom/News-Releases/2019/Diver-Survives-In-Flight-Emergency

